“At home, Nick didn’t improve. I remember he had fever but with cold hands and feet. At the time, I didn’t know these were early signs of meningitis and septicaemia. I remembered seeing a video from Meningitis Research Foundation featuring TV-doctor Dr Hilary Jones. It explained about the tumbler test and how to check if a rash was something more serious. I grabbed a glass and pressed it against the rash. I could see the marks clearly through the glass so I knew I had to get urgent medical help.”
Meningitis is difficult to spot, which means around 50% of children who have the most common type of bacterial meningitis are sent home after their first visit to a GP. It’s therefore vital for parents to trust their instincts and seek further medical help if a child’s illness gets worse. The
first symptoms are usually fever, vomiting, headache and feeling unwell. Limb pain, pale skin, and cold hands and feet often appear earlier than the rash, neck stiffness, dislike of bright lights and confusion.
Debbie drove Nick to the hospital where they confirmed he was seriously ill. The disease had progressed quickly, damaging his limbs, and the doctors warned that he would lose his hands and feet. Thankfully, the antibiotics quickly turned things around and he made a remarkable recovery.
Nick said: “I don’t remember much of it so I haven’t shared my story before. But recently I heard of someone my age with meningitis and learnt how lucky I was. When you think that one in ten will die and more than one in five have long-term effects form the disease, such as amputations or brain injury, I might not have been playing rugby today. Mum said meningitis did have an impact on me in some ways directly after I was ill – I had problems concentrating, which is a known after effect – but I had a lucky escape. I hope telling my story will help others to act quickly to get the medical help they need.”

Meningitis is spread through close contact and new figures from Public Health England Meningococcal Reference Unit show that cases of meningococcal meningitis and septicaemia dropped significantly in England and Wales during lockdown – currently at less than a third of cases compared to the same months in previous years. However, as restrictions ease, cases are expected to rise.
Nick and Debbie are supporting Meningitis Research Foundation to warn people not to be complacent. Cases are expected to rise as people socialise again, and as we move into the winter season which is when we see the peak in yearly cases. For example, MRF funded research shows that carriage rates of meningococcal bacteria in university students, one of the high risk-groups for the disease, increase rapidly in the first week of term as students begin to socialise. On the first day, 7% of students carry the bacteria, on day one, 11% on day two, 19% on day three and 23% on day four. Among students living in catered halls of residence, carriage rates reached 34% by December of the first term.
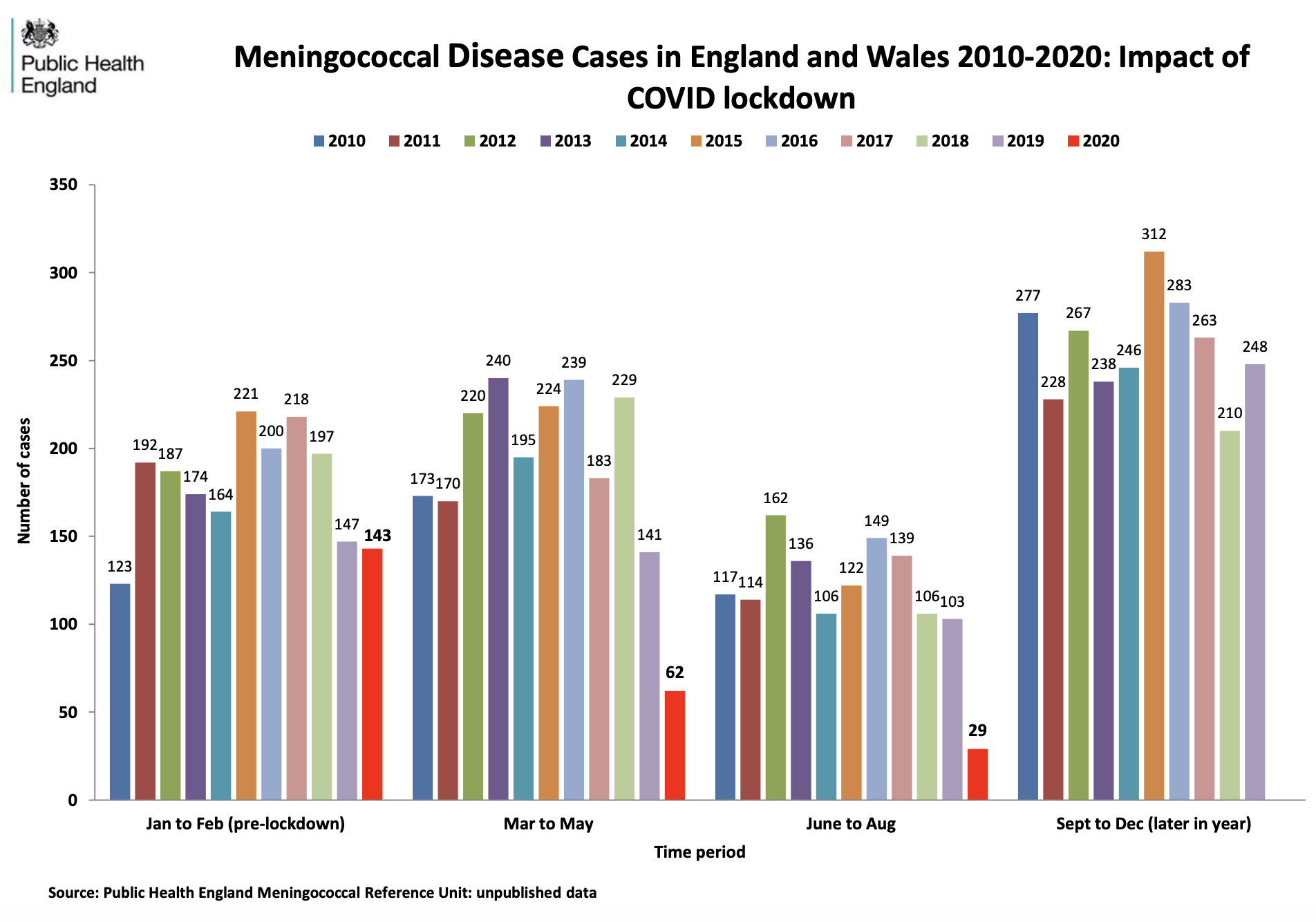
New data from Public Health England reveals the impact of lockdown on meningitis.
Rob Dawson, Director of Support for Meningitis Research Foundation, said: “Meningitis is spread through close contact. Early figures show we have seen a dramatic dip in meningitis cases in England and Wales over the last few months while people refrained from socialising, which is great news. But we cannot be complacent. Meningitis hasn’t stopped and we are expecting the next few months to see cases rise to much higher levels. Even in the midst of a COVID pandemic, urgent action against meningitis saves lives, so it’s vital people know the signs and symptoms and how to act if someone is ill. Parents can be worried about taking a child to hospital due to concerns about COVID-19, but meningitis leads to more serious illness in young children. While the country is rightly staying alert for COVID, they must also remember to think about meningitis too."