When we think of meningitis, we may think of the so-called ‘meningitis rash’ – a red or purple marking on the body which remains present when pressed with a glass. However, the rash does not always appear in cases of meningitis, and the word ‘rash’ itself may be misleading. Information and Support Officer Katherine Carter explains more.
What is the meningitis rash?
Meningitis and septicaemia can be caused by many different bugs, including viruses and fungi, but most cases of severe meningitis and septicaemia are caused by bacteria. Meningococcal bacteria in particular are the most common cause of the meningitis rash.
These bacteria can be very common and are mostly harmless, but in some people this bacteria invade the body via the back of the nose and throat, causing severe illness and even death. Sadly we don’t yet understand why some people get ill from a bacteria that is harmless to most of us.
Once the bacteria have invaded the back of the nose and throat, they travel through the bloodstream. As this happens, the bacteria rapidly multiply and produce toxins which travel around the body causing damage to blood vessels and organs. As the blood vessels get damaged, blood starts to ‘leak’ into the surrounding tissue, often causing what looks like a ‘rash’ to appear on the skin. However, this does not always appear.
What does the rash look like?
This rash can be one of the clearest and most specific signs of meningococcal meningitis and septicaemia to recognise – hence why you have probably heard of it. However, meningococcal rashes can be extremely diverse, and look different on different skin types. The rate of progression can also vary greatly.
- A petechial rash looks like pin-prick red or purple spots on the skin, and can resemble flea bites.
- A purpuric rash looks more like bruising, showing up as reddish-purple areas on the skin.
A rapidly evolving petechial or purpuric ‘rash’ is a marker of very severe disease. As part of the MRF helpline team, I have had a parent describe a rapidly evolving rash as “like someone using a biro to draw all over the skin”. If you, or someone you know, appears to be suffering from a rash of this kind, please seek medical help immediately.
Isolated and dispersed pin-prick spots may first appear, so it is important to search the whole body for small petechiae, or red and purple spots. Petechiae are 1 to 2 mm in diameter and commonly appear in clusters in areas where pressure occurs from elastic in underwear, nappies or stocking. The rash can be more difficult to see on dark skin, but may be visible in paler areas, especially the soles of the feet, palms of the hands, abdomen, or on the inside of the eyelid or roof of the mouth.
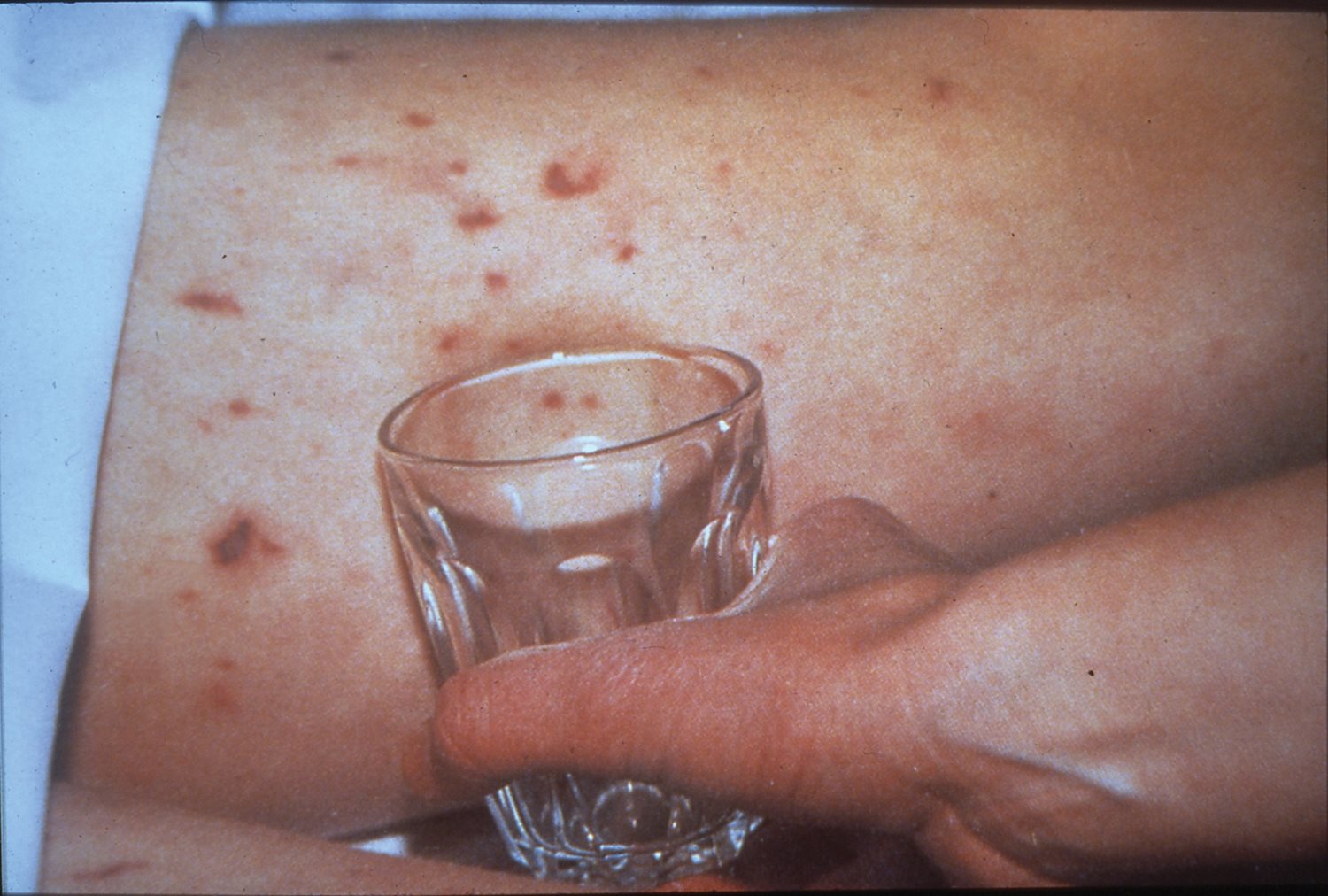
The 'glass test' can be used to determine if a rash is or is not a symptom of meningitis.
What does the ‘glass test’ do?
Many people are familiar with the so-called “tumbler test” or “glass test”, whereby a glass or other clear surface is pressed onto the rash. If it disappears when pressed, this is known as a blanching rash. The meningitis “rash” can start as a blanching rash, but nearly always develops into a non-blanching red, purple or brownish petechial rash or purpura, meaning it will not disappear when pressed.
What might happen after the rash has appeared?
In response to the blood vessels leaking as the disease progresses, the body produces an overwhelming clotting response, which stops oxygen from reaching the extremities. This results in extensive purpuric areas, usually called ‘purpura fulminans’, which look like large bruises over the skin and can be very dark in colour.
The extremities are normally worst affected: often the feet and hands (but can extend over a whole arm or leg) and sometimes the ears, nose or lip. Devastatingly, as the extremities become starved of oxygen, they can become blackened which can lead to scarring and amputation.
What should I do if someone has lots of other meningitis symptoms, but no rash?
Most patients with overwhelming meningococcal septicaemia develop a rash - it is one of the clearest and most important signs to recognise. However, in cases of meningitis the rash can be very scanty, blanching, atypical or even absent. When we talk about meningitis, we often think ‘rash’, but it is incredibly important to know that a rash won’t always appear.
Please remember that a very ill person needs medical help even if there are only a few spots, a rash that fades, or no rash at all. Trust your instincts, someone who has meningitis or septicaemia could become seriously ill very quickly. Get medical help immediately if you suspect meningitis or septicaemia – rash or no rash!